Life
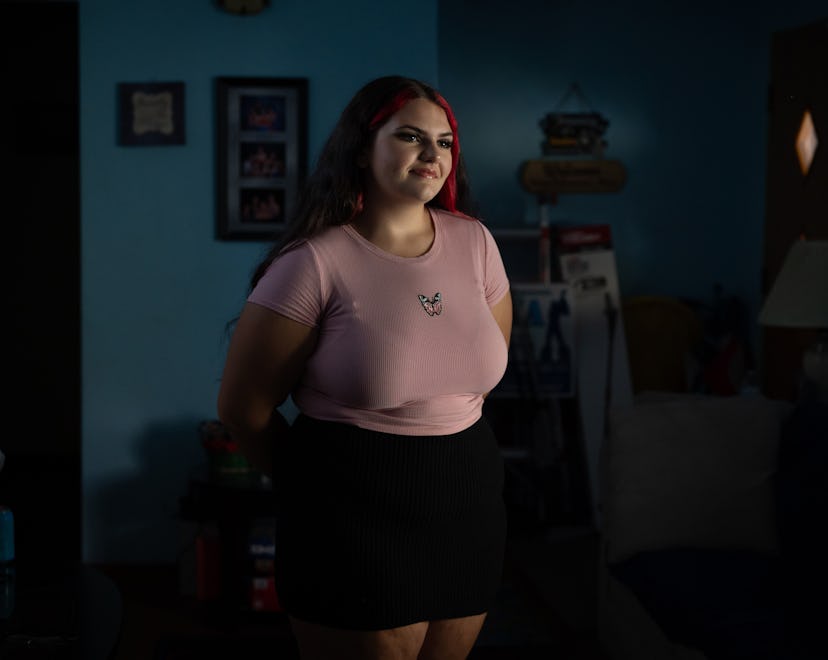
We Need To Talk About Teens & Weight-Loss Drugs
Wegovy is now approved for use in kids as young as 12. But will it do more harm than good?
Emmalea Zummo was the teen face of the weight-loss drug Wegovy. In November 2022, after a study in the New England Journal of Medicine revealed the weekly injection was highly effective in helping adolescents in the 95th weight percentile shed pounds, a then-17-year-old Emmalea appeared on NBC Nightly News to sing the drug’s praises.
While participating in the study, she lost 70 pounds, she said, and gained confidence after years of being teased by her classmates for her body size, which had expanded after developing the hormonal disorder polycystic ovary syndrome, or PCOS.
“I tried diets. I tried exercise. I’m in more sports than any other kid I know, and nothing would work,” Emmalea told NBC. Her weight made her feel hopeless, she said, and she became depressed. Then she took Wegovy, and her outlook transformed. “I lost the weight, but I also lost the dread,” she said. “It was like a weight off my back and my stomach.”
Emmalea had learned about the drug trial from the doctor who was treating her PCOS, who co-authored the study; she told Emmalea she was a good candidate, since weight loss can help lessen some symptoms. The teen then made the case to her mother, Davina Zummo, who was supportive. “For Emmalea, the end goal,” her mother tells Romper, was to “feel more confident and be able to be more active without injuries and issues that extra weight can cause. That was enough for me to say OK.”
“I lost the weight, but I also lost the dread.”
But the nearly 16 months Emmalea spent on Wegovy for the clinical trial were only the beginning of her experience with the medication, both physically and emotionally. After the study ended and the NBC interview aired, Emmalea, who is now 18, wasn’t able to afford the medication — which has a list price of $1,300 per month — despite working two jobs in her hometown of Jeanette, Pennsylvania. Her parents’ insurance did not cover it. By early this year, she had gained back most of the weight, which led her to develop an eating disorder.
“The medication worked very well for me,” she says. But since the drug trial ended, she’s weathered “a lot of stress and strain.” Davina says it was “gut-wrenching” to watch her daughter beat herself up as the number on the scale increased.
Emmalea’s experience offers a window into just a few of the complex challenges that mental health experts say are being overlooked in the cultural enthusiasm about Wegovy, a brand name for semaglutide, which physicians, media outlets, and celebrity influencers alike are touting as a near-miracle drug that is poised to usher in a paradigm shift in how we think about body size.
“The conversation on the Internet has been really one-sided towards the positives of this medication,” says Natacha Emerson, Ph.D., a psychologist at the University of California, Los Angeles’ pediatric obesity clinic. But “we’re not really considering the entire picture.”
Like body size and weight, the drug’s appearances can be deceiving.
Why are teens taking Wegovy?
Wegovy has only been available to kids ages 12 to 17 since December 2022. Since then, interest has surged, according to the adolescent mental health professionals Romper interviewed. “In the last few months, we’ve had this major shift,” says Emerson. “More and more, we’re having teenagers who are coming in seeking medications.”
Semaglutide was initially developed to treat Type 2 diabetes in adults but is now marketed and sold specifically for weight loss. (Ozempic also contains semaglutide, but at a slightly lower dose.) In addition to prompting the body to produce more insulin, which lowers blood sugar, the drug releases a hormone that makes you feel fuller faster while eating; it also causes the stomach to empty more slowly, which contributes to a feeling of satiety.
But Wegovy is not without side effects. It’s common for people who take semaglutide to experience nausea, diarrhea, headaches, and fatigue. For Emmalea, “the biggest thing was the stomach cramps,” says Davina, her mother. The aching eventually went away as her daughter’s body adjusted to the drug, but for others, side effects persist.
Still, late last year, the Food and Drug Administration approved Wegovy for adolescents in the 95th or greater weight percentile for their age, sex, and height, based largely on the results of the drug trial in which Emmalea participated, which was funded by drugmaker Novo Nordisk. (It’s common practice for pharmaceutical companies to fund trials for their own drugs.) The study found that participants who received a weekly injection over roughly 16 months lost an average of 14.7% of their starting body weight.
“We’re more likely to target true concerns when we aren’t using weight as a proxy for health. Shame and stigma does not improve health.”
A few weeks after Wegovy’s approval, the American Academy of Pediatrics released its new official guidelines for evaluating and treating kids deemed obese and gave the notion of prescribing weight-loss drugs to kids a boost: For the first time, the academy said there was evidence that weight-loss medication was an appropriate treatment for some adolescents who haven’t been able to lose weight through changing their diet or increasing their physical activity, clearing the way for doctors to prescribe them.
The guidelines are based on research suggesting that being a certain weight — or more specifically, having a high body mass index — is correlated with a higher risk of developing a host of serious medical conditions, including Type 2 diabetes, non-alcoholic fatty liver disease, and cardiovascular disease, and the earlier doctors can intervene and assist kids in lowering their BMI, the better they’ll be able to prevent these issues from happening.
This was a dramatic escalation of earlier recommendations, which promoted simple lifestyle changes and encouraged more of a wait-and-see approach.
“A lot of pediatricians don’t think about the long-term implications of their neglect of individuals that have obesity,” says Dr. Fatima Stanford, M.D., an obesity medicine specialist at Massachusetts General Hospital and Harvard Medical School, who reviewed early drafts of the American Academy of Pediatrics’ obesity guidelines. “Because let me tell you, they come to me as adult patients, and they always hearken back to what their pediatrician did or did not do — and often it is what they did not do to help them to live their best life.” (Stanford has consulted for companies developing weight-loss drugs.)
And yet, the recommendations have come at a moment when the very premise that obesity is a disease is being challenged, and when mounting evidence suggests that while weight and body fat can contribute to certain health conditions, there is far from a direct causation for everyone.
“For any given patient, we have no idea whether somebody’s BMI is going to be associated with the development of diabetes or the development of coronary artery disease,” says Dr. Kimberly Dennis, M.D., a psychiatrist and the co-founder of SunCloud Health, an eating disorder treatment center in the Chicago area. “Being in a larger body is not an illness.”
Over the past few years, a growing number of clinicians have begun promoting Health at Every Size, an approach to care that counters conventional wisdom that body size and weight are, in and of themselves, problems to be solved.
“It’s hard to see what we lose by not pathologizing larger bodies,” says Virginia Sole-Smith, the author of Fat Talk: Parenting in the Age of Diet Culture and the diet-culture newsletter Burnt Toast. “We can still prescribe medications that treat health concerns, and we’re more likely to target true concerns when we aren’t using weight as a proxy for health. Shame and stigma does not improve health.”
“Being in a larger body is not an illness.”
This conundrum has not been easy for parents to navigate, Dennis says. “I feel for families who are going to doctors terrified about their kid being stigmatized for the rest of their life because of their weight, or terrified of their kid developing diabetes or having some other health consequence that, again, they may never have, ever. So it puts families in a really impossible situation, too.”
For Davina and Emmalea Zummo, the potential risks of not losing weight trumped the potential dangers of taking a drug. Davina says she saw Wegovy as a way to help her daughter “essentially get healthier,” she says, and to help protect her against future diseases that could require even more medication as an adult. Of course, the promise of watching her clothing size decrease was a powerful incentive, too.
“Kids are mean,” Davina says. “It doesn’t matter how hard you work, how good you look, how positive you are, how anything — kids are mean. Emmalea put on a brave face, but it did affect her.”
‘We don’t want young people avoiding food.’
The mental health professionals we spoke with for this piece shared a long list of concerns about teens taking Wegovy, most of which boil down to the fear that medicating kids who don’t necessarily need to be medicated — and with a new drug that hasn’t seen any long-term testing, which one must take indefinitely for it to work — may do more harm than good, both physically and psychologically.
If an adolescent has already developed prediabetes, hypertension, or other diseases correlated with weight, Wegovy may be an appropriate treatment, most of the professionals agreed, but they urged caution in prescribing the drug to young people based on body size or BMI alone. It’s this potential use of the drug — as a way to, theoretically, make life easier for young people by helping them lose weight and remove the target off their backs as they make their way through a deeply fat-phobic world — that raises more questions than it answers.
“My biggest concern is that nobody who prescribes these drugs is accompanying that prescription with an in-depth exploration of how anti-fat bias is making this teen’s life harder and health worse,” Sole-Smith says. “I’m certainly not against kids taking a medication that can improve their metabolic health. But when it’s marketed and prescribed as a weight-loss drug, we’re telling kids that their weight is the problem.”
Charlotte Markey, Ph.D., a professor of psychology and chair of the Health Sciences Department at Rutgers University, Camden, agrees. “Physicians receive very limited training in terms of how to talk with patients about weight, body image, and eating disorders,” she says. And so, “I worry that physicians aren’t equipped to even bring up this conversation without really negatively impacting youths’ body image. The suggestion that a medication is needed because your body is not alright as it currently is is a pretty powerful and demoralizing message.”
Dennis suggests it’s also an unethical one. “Are we thinking, ‘Here’s this medication, take it for the rest of your life, and take it because you’re in a larger body’? That just seems like quite a sentence to be handing down to somebody whose identity is still in the process of developing.” (Since the American Academy of Pediatrics guidelines were released last January, the National Eating Disorders Association has partnered with the organization and others to create a work group, of which Dennis is a member, to better address the mental health effects of caring for kids in larger bodies.)
“I’m not against kids taking a medication that can improve their metabolic health. But when it’s marketed and prescribed as a weight-loss drug, we’re telling kids that their weight is the problem.”
Stanford points out that doctors often prescribe young people medications meant to be taken indefinitely, when the benefit outweighs the risk — for asthma, for example, or diabetes, or attention-deficit/hyperactivity disorder, or a long list of other health conditions. But making that determination with Wegovy can be challenging for doctors, parents, and teens alike. Nearly every expert we spoke with pointed out that the promise of quick and dramatic weight loss may be enticing to adolescents growing up in a culture that prizes thinness, but teenage brains are wired to take short-term risks without fully appreciating long-term consequences.
“Teenagers in general — and this is well-established — don’t have a fully developed frontal lobe. They have this tendency to really overemphasize any benefit of risky actions,” says Emerson. “And so, a lot of the teenagers we’re seeing have this fantasy that once they’re thin, everything else in their life will fall into place.”
Emerson expressed concern that taking Wegovy could serve as a kind of superficial bandage to underlying mental health issues such as anxiety, depression, and poor self-esteem, treating the symptom but not the cause. “Having the body that you want does not necessarily mean that it’s going to erase your depression, your anxiety, your low self-esteem,” she says.
Eating disorder specialists also point out that kids in larger bodies are at higher risk for developing disordered eating and full-scale eating disorders, and exposure to Wegovy could increase that risk. But even if teens don’t develop an eating disorder, Wegovy could complicate their ability to develop a healthy long-term relationship with food. “We don’t want young people avoiding food. We want them attending to the natural signals their bodies produce to let them know they are hungry and full,” says Markey.
While this is also important for adults, she says, it’s particularly vital for adolescents who are still growing. “Taking a medication that tamps down their hunger is not exactly a great way to ensure that growing bodies get the nutrition they need for pubertal and brain development,” she says.
“Having the body that you want does not necessarily mean that it’s going to erase your depression, your anxiety, your low self-esteem.”
While most pediatric obesity specialists require patients on Wegovy to work closely with a nutritionist to make sure they are eating enough nutrient-dense foods to support their growth and development, without this guidance, there “is potential for undernutrition … that could theoretically lead to specific nutritional deficiencies,” says Dr. Richard Chung, M.D., an adolescent medicine specialist at Duke University Medical Center.
Wegovy may be portrayed as a quick and easy fix to teens’ body angst in popular media, but for most adolescents, it’s neither.
What happens when you stop?
Young people who don’t like the way Wegovy makes them feel can theoretically stop taking it at any time, but clinical trials show that, when they do, they are likely to gain back the weight they lost. Some people have been forced to stop for other reasons: Semaglutide’s surging popularity has led to shortages of the drug, and many, like Emmalea, can’t afford it without insurance coverage.
Experts were particularly concerned about the risks of “weight cycling,” or losing and regaining weight, which research suggests not only slows down the body’s metabolism but also stresses the cardiovascular system. “Weight cycling has really negative consequences for health,” says Markey, and “starting Wegovy or a similar drug in your teens means you could have … a life of weight cycling ahead of you.”
Not only could starting and stopping Wegovy negatively impact kids’ metabolism into adulthood, say the experts we spoke with, but it also could lead to emotional whiplash. “It’s a big experiment” at this point, says Dennis. (Research has not shown that semaglutide itself negatively impacts kids’ metabolism.)
Starting and stopping Wegovy could “snowball” any potential mental health side effects. “Let’s say you have a kid who’s already at high risk for depression and anxiety; perhaps they’re picked on, or they don’t have good body image,” Emerson says. “They get on the drug, they have this sense that it’s going to cure everything, they do have some weight loss, but lo and behold, they also have other side effects that are unpleasant and for which people discontinue use quite frequently.” If they stop using it and regain weight, she says, they could “be in a worse place mentally than when they were when they started.”
This was the case for Emmalea Zummo.
For the first three months after she stopped taking Wegovy, Emmalea felt good. She continued to eat balanced, nutritious meals and exercise often. But as her appetite gradually increased and the number on the scale crept back up, she began to starve herself by skipping meals. She would then become so hungry that she would binge eat. “It was a very unhealthy cycle,” she says.
She’s in a healthier place today, she says, thanks to the support of her parents and a therapist, but staying there requires constant mental, emotional, and physical effort. “I have mostly recovered,” she says. “Obviously, there are things that you have to fight daily. You have to keep a positive mind space. But I have gotten through the roughest part of it.”
Novo Nordisk told Romper in a statement that the company cannot comment on individual cases, explaining, “We trust that health care providers are evaluating a patient’s individual needs and determining what treatments or interventions are right for that particular patient… A return of signs/symptoms is the likely result when successful treatment is discontinued. ”
Despite everything she’s been through, Emmalea is eager to start taking Wegovy again. While I was reporting this story, her parents’ insurance agreed to cover it, but she has been unable to start up again due to a national shortage. Davina supports her daughter going back on the drug. “Yes, we did go through issues, but I think she’s worked through those,” she says. “She’s where she needs to be.”
Knowing what she knows, and living through what she has, Emmalea believes the medication is the right choice for her specific set of circumstances. She says she can’t predict whether in 10 years she will regret it. Nor can any of the families considering Wegovy — hoping for a better future for their kids, venturing into a murky unknown.
If you or someone you know has an eating disorder and needs help, call 988 or text “NEDA” to 741741 to be connected with a trained volunteer at Crisis Text Line. Another resource is the Alliance for Eating Disorders.
Danielle Friedman is an award-winning journalist who focuses on the intersection of health, sexuality, and culture. Her first book, Let’s Get Physical: How Women Discovered Exercise and Reshaped the World, came out in early 2022. Her writing has appeared in The New York Times, New York Magazine’s The Cut, Vogue, Glamour, Harper's Bazaar, the Washington Post, NBC News, InStyle, The Daily Beast, Health, and other publications.
Previously, she has written for Romper about how to reframe your relationship with exercise and how Title IX changed the world for girls.
Photographs by Stephanie Strasburg
Photo Director: Alex Pollack
SVP Creative: Karen Hibbert
This article was originally published on