Life
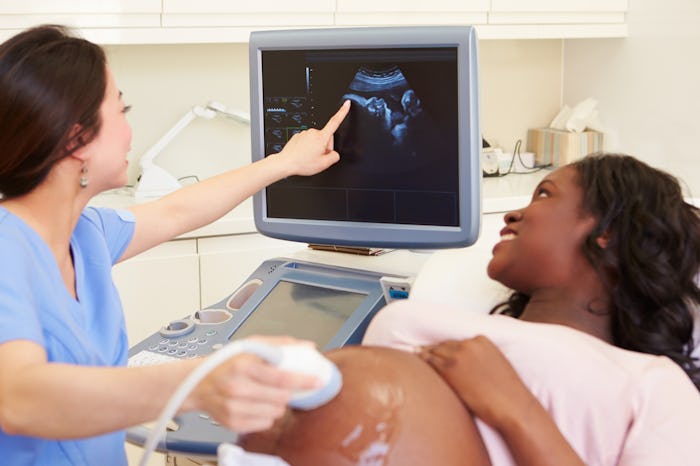
Here's Why Experts Say You Shouldn't Worry About Ultrasounds Being Harmful
Why is it that so much of the conversation surrounding pregnancy seems to include a lot of talk about too much/too little? Am I exercising too much? How much Brie can I really eat? Are too many ultrasounds harmful? It's a lot of back and forth, to say the least. Of course blood tests, cervical checks, heartbeat monitoring, and ultrasounds alleviate some of that concern, but that latter question can really throw you for a loop.
“I am frequently asked if ultrasound during pregnancy is safe," Dr. Sherry Ross, an OB-GYN and women’s health expert at Providence Saint John’s Health Center in Santa Monica, California, tells Romper in an email interview. "Pregnant women can take a sigh of relief knowing that there is no evidence showing that ultrasound is harmful to a growing baby at any stage of pregnancy."
Ross explains that ultrasounds are simply high frequency sound waves that are used throughout pregnancy to evaluate the growth and health of a fetus, as well as to look at the ovaries, placenta, and amniotic fluid. "There is no scary radiation being transmitted during ultrasound," she says.
Dr. Allison Hill, OB-GYN and author of Your Pregnancy, Your Way, agrees, adding that ultrasound, which has been used for medical purposes since the 1950s, does not contain radiation like that found in X-rays or CT scans.
"The safety of ultrasounds has been well established," Hill tells Romper in an email interview. "A review of over 50 medical studies shows that ultrasounds do not pose any danger to moms or fetuses. They do not cause birth defects, childhood developmental or intellectual problems, or cancer."
Hill says that skeptics point to animal models in which an increase in fetal temperature from the ultrasound waves has been related to birth defects. "However, the temperature would need to increase by at least 1.5 degrees, which would require over four hours of continuous ultrasound exposure," she says. "It is unlikely that the routine ultrasounds done during pregnancy — which last 15 minutes or less — could cause harm. These findings from animal models have never been seen in humans."
Ross says ultrasounds are performed in the first trimester to evaluate an early pregnancy and establish the dating of the pregnancy. You can also count on an ultrasound between 16 and 20 weeks to assess the structural anatomy of the fetus as well as its sex (if you want to find out). "From a doctor’s viewpoint, ultrasound is a helpful set of eyes making sure your growing baby is healthy."
Hill says some high-risk pregnancies do require more ultrasounds. That means moms-to-be with chronic conditions like type 2 diabetes, high blood pressure, lupus, or growth-restricted fetuses might require more frequent scanning, according to What To Expect.
"For some mothers, having multiple ultrasounds instills fears about their pregnancy: the baby looks too big, the baby looks too small, the baby has the cord around its neck (actually a normal finding)," Hill says. "Or maybe there was just 'limited visualization,' meaning some of the organs couldn’t be evaluated completely because of the size or position of the baby. In the mom’s mind, these results translate to 'there may be a problem.'"
That's where fluid conversation between a soon-to-be mother and her healthcare provider is crucial, says Dr. Vasiliki Moragianni, a board-certified OB-GYN and reproductive endocrinologist with Colorado Center for Reproductive Medicine in Northern Virginia.
"The most critical component of the patient-physician relationship is an open two-way communication," she tells Romper in an email interview. "Whenever a patient is concerned about an issue, such as pregnancy ultrasound frequency, she should feel comfortable enough to discuss it with her physician. Otherwise, a therapeutic relationship cannot be established and alternatives should be explored."
One related issue you might be wondering about is the difference between "regular" 2D ultrasounds and ultrasounds in 3D and 4D. As What to Expect explained, these are generally "performed only to closely examine suspected fetal anomalies, such as cleft lip and spinal cord issues, or to monitor something specific. In other words, 3D sonograms and 4D ultrasounds are not part of routine prenatal exams." If your doctor deems a 3D or 4D ultrasound necessary, there's no cause for concern over the procedure's safety. That said, the Food & Drug Administration (FDA) and the American Congress of Obstetricians and Gynecologists (ACOG) "say that ultrasounds should only be performed by a qualified medical professional when your practitioner deems them necessary for medical reasons," according to What to Expect. That means studios and mall kiosks offering "the use of any kinds of ultrasounds (2D, Doppler, 3D and 4D) for the purpose of creating a memento" should be avoided:
"In addition to potentially putting your baby’s health at risk, the technicians who perform commercial ultrasounds may not be able to address your questions and likely won’t have the expertise to be able to spot any problems with your baby’s development. What's more, some commercial sessions last for 45 minutes — much longer than a medical scan. A long session (or repeat sessions, as some of these centers offer) can be intrusive and disruptive for a fetus who's using womb time to grow, develop and get the sleep he needs."
Just remember, you'll be seeing your little one's face in person before you know it... and the wait will be *so* worth it.
Experts:
Dr. Sherry Ross, OB-GYN
Dr. Allison Hill, OB-GYN and author of Your Pregnancy, Your Way
Dr. Vasiliki Moragianni, a board-certified OB-GYN and reproductive endocrinologist
This article was originally published on