Life
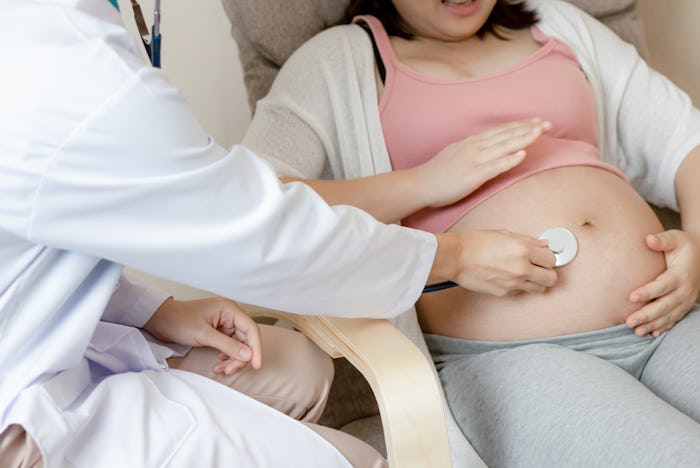
How Coronavirus Affects Your Birth Plan
A little (or a lot of) planning before your due date helps ease some of the stress of giving birth, but some things are harder to plan for. The novel coronavirus is now responsible for more than 5,000 cases of COVID-19 in the U.S. and counting. The reality is that you or someone you know might be giving birth during the coronavirus pandemic. While expecting families can check their hospital bag and the car seat as many times as humanly possible, planning for birth in these next few weeks requires a little bit more awareness.
Because the respiratory disease COVID-19 is new, experts are still trying to find out more about it. The uncertainty surrounding this novel coronavirus is understandably scary, especially for groups such as moms-to-be. What we do know, according to the CDC, is that coronaviruses usually spread when an infected person coughs or sneezes and the droplets land on a surface or directly into the mouths or noses of nearby people. Any direct contact, such as shaking hands with an infected person and then touching your mouth, nose, or eyes can also transmit COVID-19. What does this mean for pregnant women with upcoming due dates?
Currently, there’s not enough information regarding whether COVID-19 specifically poses a greater risk to pregnant women. Researchers do know that viruses in the same family as coronaviruses, such as influenza, affect pregnant women more severely than they do the general population. But so far, there’s no evidence to suggest that women diagnosed with COVID-19 can pass the disease to their baby in the womb or during childbirth. “For mothers that have been found positive, at this time there has been no vertical transmission, meaning there hasn’t been any virus found in the amniotic fluid, and positive mothers have not given birth to neonates that are positive,” says Dr. Sanlare C. Gordon, obstetrician and gynecologist specializing in high-risk pregnancy at Anne Arundel Medical Center and host of pregnancy podcast the Mature Momma Life.
Dr. Gordon encourages parents concerned about their baby becoming infected after birth to find out what their hospital is doing to prevent the spread of coronavirus. “Patients should only be concerned if they are in a hospital system that isn’t properly screening patients,” she says. “Hospitals are doing an incredible job in screening people to make sure they aren’t spreading the virus.” She explains that labor and delivery floors are considered non-infectious areas of the hospital, and moms giving birth shouldn’t expect to come into contact with the general hospital population. “Pregnant patients are considered immunocompromised, so we try to keep these areas free from viruses such as influenza, active tuberculosis, and now coronavirus,” she says.
Women with upcoming due dates can also expect some significant changes at the hospital. Those who have scheduled cesareans or inductions should check with their hospital to find out about being screened for COVID-19, which Dr. Gordon says should occur at least 48 hours before coming into the hospital. Hospitals are also limiting the number of visitors, so it’s a good idea to call or check your hospital’s website to find out the specifics of the limits. Maternity ward tours and classes, such as prenatal and Lamaze classes, are moving online. All of these restrictions are to limit the possible exposure of the novel coronavirus to patients. Although the American College of Surgeons has recommended doctors reschedule all elective and diagnostic surgeries, both scheduled and emergency c-sections are not expected to be affected as they’re not considered elective.
As far as staffing on labor and delivery floors, pregnant women shouldn’t worry that their birth will turn into a scene out of Grey’s Anatomy. “Obstetrical nurses will not be asked to go to floors to help with COVID-19 patients. They should be available, and not pulled to give care to people off of the labor and delivery floor,” Dr. Gordon says. “We are trying to reduce spread, so introducing more essential healthcare providers to the virus would not help to flatten the curve.”
Ultimately, the main goal for pregnant women should be to stay healthy. The World Health Organization (WHO), the CDC, and public health experts strongly encourage social distancing — avoiding crowds, public spaces, and gatherings. For pregnant women that also means avoiding contact with people outside of the immediate family. “Pregnant patients should avoid gatherings larger than 20 people, nursing homes, hospitals, and people that admit to flu-like symptoms. They should also avoid airline travel as it has been reported that infected persons are knowingly traveling,” Dr. Gordon says. Practicing good hand-washing and sanitizing household surfaces are also the best ways to prevent the spread of coronavirus, she says.
The current data doesn’t give us a completely clear picture of how the novel coronavirus impacts pregnant women. It’s unclear whether COVID-19 can cause preterm birth or whether it causes any long-term effects to babies who test positive, according to the March of Dimes. If a pregnant woman is found to be positive, she will be quarantined and monitored closely per the hospital’s policies, says Dr. Gordon.
A report published recently in Frontiers in Pediatrics studied four women infected with COVID-19 when they gave birth. Three of the babies were born via cesarean section and one was born vaginally. All four babies were born without symptoms of the virus, including fever and trouble breathing. Of the babies who were tested for COVID-19 (mom declined testing for one), all tested negative, suggesting that transmission of the novel coronavirus does not occur in the womb or through the placenta.
Two cases, one in London and one in China, suggest that transmission immediately after birth, however, is possible. In February, a mother and her newborn baby tested positive for COVID-19 minutes after birth in Wuhan. The BBC reported that medical professionals were still investigating how the baby contracted the virus, but believe it might have been by inhaling the mom’s droplets after coughing. Another more recent case in London resulted in a similar response from medical professionals who were unsure if the baby contracted the virus during or after birth.
If you have symptoms, including fever, shortness of breath, and cough, please call your obstetrical provider for guidance. With so many unknowns, avoiding panic and taking the precautions recommended by the CDC to avoid infection is the best course of action for women counting down their due date in the thick of the coronavirus pandemic.
If you think you’re showing symptoms of coronavirus, which include fever, shortness of breath, and cough, call your doctor before going to get tested. If you’re anxious about the virus’s spread in your community, visit the CDC for up-to-date information and resources, or seek out mental health support. You can find all of Romper’s parents + coronavirus coverage here, and Bustle’s constantly updated, general “what to know about coronavirus” here.
Experts:
Dr. Sanlare C. Gordon, DO, obstetrician and gynecologist at Anne Arundel Medical Center and host of pregnancy podcast the Mature Momma Life
Studies referenced:
Chan, Y. et al. (2020). Infants Born to Mothers With a New Coronavirus (COVID-19). Frontiers in Pediatrics. https://www.frontiersin.org/articles/10.3389/fped.2020.00104/full