Life
Here's What Med Students Actually Learn About Pregnancy — And What They Don't
By the time a pregnant woman has her baby, she is likely to have become a partial expert in topics like c-section interventions, preeclampsia, analgesia, episiotomies, skin-to-skin contact, cervical effacement, hep-locks, caffeine consumption, and the perils of brie, to name just a few. Still, many expecting moms will find conflicting information between the advice offered in books and that given by their OB-GYNs, or the American Congress of Obstetrics and Gynecology (ACOG). These differences of opinion can complicate decision-making for pregnant women and potentially impact the trust between patient and doctor. And that begs the question: What exactly do medical students actually learn about pregnancy in medical school? And, perhaps just as important, what do they not learn?
To get the answers, Romper reached out to medical students and doctors to find out more about the baseline training in pregnancy, labor, and delivery that’s common in medical schools. At this stage, pregnant people are rarely involved; class involves cadavers, mannequins, and standardized patients trained to "present" as pregnant.
Because pregnancy impacts all the body's systems, students must study cardiology, endocrinology, and pulmonology, for example, leaving less time for topics like breastfeeding, pain-free delivery and so on. “Pregnancy is really complicated,” says Zoe Kornberg, a third-year medical student at UCSF School of Medicine who is considering specializing as an OB-GYN, explaining that it requires a solid base in physiology.
The in-class curriculum includes things like how the reproductive system works, how conception happens, embryo and fetal development, the stages of pregnancy, what tests should be ordered and when, what issues to monitor, and common conditions and how to treat them. They also learn about the stages of labor and delivery, along with what can go wrong and when certain interventions, like c-sections, are recommended.
Most medical students also spend time in the cadaver lab. “We get to dissect cadavers and look at their reproductive organs,” Kornberg says. “You look at every aspect of them. You see how big they are. You see how stretchy they are. Those are things that are so important to understanding how a fetus can fit inside someone or how a fetus can fit through the pelvis at delivery.”
Although cadavers tend to be older people — and not pregnant — Kornberg says that some of the cadavers she examined were women of childbearing age. Every year, UCSF holds a vigil to thank the people who donated their bodies to the medical school.
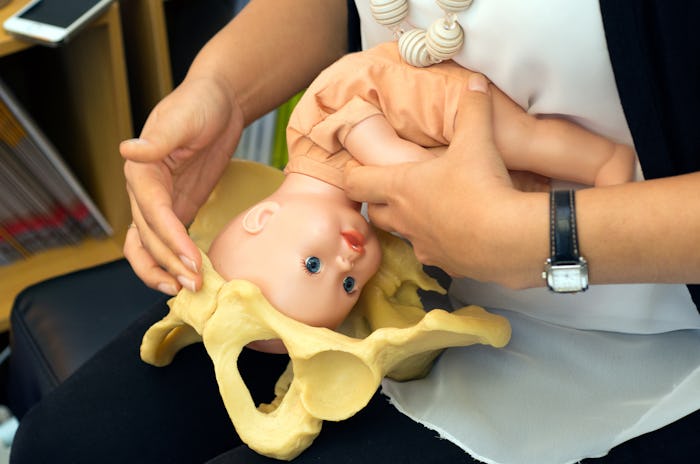
Medical students also need to learn practical skills, such as how to do a pelvic exam, and usually mannequins are the starting point. These mannequins, which are often just the lower torso and upper thighs, are designed specifically for teaching pelvic exams, explains Claire Bodkin, a second year medical student at McMaster University’s DeGroote School of Medicine, in Hamilton, Ontario.
“It’s supposed to be realistic, but it’s pretty rigid. I would not describe it as lifelike although I think it attempts to be lifelike,” Bodkin laughs. Even so, she’s glad she had a chance to practice on a mannequin first before examining a patient. “It’s really nice to go through the motions even just to figure out where you want your lighting and how to hold the speculum.”
Mannequins may not be perfect, but they’re better than some disturbing alternatives from the recent past. For years, it was common for medical students to practice pelvic exams on anesthetized women prior to gynecological surgery, without their explicit consent. As recently as 2012, a medical student complained about being asked to do this. Professional medical organizations, like ACOG, now have guidelines requiring informed consent, and the practice seems to have stopped.
Fortunately, there are better ways for medical students to get experience doing exams on real people. Most medical students have opportunities to learn on “standardized patients,” or people who are trained to teach the exam using their own bodies. At UCSF, Kornberg learned from a company called Project Prepare, which operates with the goal of teaching students to perform “comfortable and effective genital exams.”
The educators explain how to do the exams and then act out different scenarios. As the students practice, the educators provide feedback and guidance. “They’re so incredibly forgiving and understanding,” Kronberg says, since learning to perform a pelvic exam can be awkward. “You’re trying to be respectful, trying to go slowly, but at the same time, to be reassuring and professional.”
“The mannequins are pretty good,” she adds, but notes that it’s not the same as learning to feel the different sensory elements of the exam on a person. “There’s just nothing like the real thing.”
Looking back, it’s really just a broad view and they’re trying to give you the bread and butter of the most common things. Unfortunately certain things just don’t [make the cut]. There is no time.
In the last two years of medical school, students start working with patients. Training usually includes 6-week rotations in obstetrics and gynecology and in family medicine, among other areas. During Kornberg’s OB-GYN rotation, she went to the same hospital every day, and learned from attending physicians, residents, midwives, and nurses in labor and delivery, gynecologic surgery, and an outpatient clinic. During the day, she could be present for anything from a fertility appointment to prenatal care to a birth. Students spend much of their time observing the medical team and patients, and learning the right questions to ask, Kornberg says. At night, students research issues that came up during the day and study for the standardized exam that comes at the end of the rotation.
It’s far from easy. But, despite the overwhelming amount of material covered in medical school, there’s always more to learn. And you may be surprised by some of things that get left out.
“When you’re in medical school, it seems like you’re learning all the detail. It seems like they want to teach you everything,” says Dr. Janet Zhao, a family doctor and mom in London, Ontario, who graduated from medical school in 2013. “But now looking back, it’s really just a broad view and they’re trying to give you the bread and butter of the most common things. Unfortunately certain things just don’t [make the cut]. There is no time.”
That includes lots of issues that make the cover of pregnancy magazines or fill whole chapters of pregnancy books. If you’re pregnant, some of the topics that you spend hours Googling may only be covered in a brief, cursory way in medical school: Think birth plans, pain management, unmedicated birth, labor positions, high c-section rates, the role of midwives and doulas, and breastfeeding. These are topics that doctors tend to learn more about through self-study or during residency, which adds years of additional training.
It means there may be a disconnect between what a pregnant person expects their doctor to know and the doctor’s initial training.
“There is so much to learn and there’s not enough time for everything,” Zhao explains. And for doctors who don’t want to become family physicians or OB-GYNs, the information may not be useful. “I wouldn’t expect all med students to have such a keen interest for obstetrics just like I have no interest at all in learning about surgery,” she adds.
But it means there may be a disconnect between what a pregnant person expects their doctor to know and the doctor’s initial training. Since medical students have volumes to learn in a short time, it makes sense that there’s more emphasis on knowledge and skills that save lives.
Zhao notes that she occasionally comes across people who worry that giving birth at a hospital is unsafe or that doctors are intervening too much in what’s supposed to be a natural process. But, she says, “We have seen as doctors that things can go really wrong. Yes, delivering a baby is natural but it can also be fatal, and historically, it often was.”
The other side of the issue is that, with so much focus on risky complications, medical students may miss out on learning about important wellness practices, like breastfeeding.
“Because there is so much for us to learn in medical school, we don’t really learn a lot about the normal stuff, about how to manage the things that are not super dangerous,” says Dr. Brenna Velker, a family physician in London, Ontario, and mother of twins.
Velker experienced this firsthand after her own difficult pregnancy. Her twins were born prematurely, at only 30 weeks. Her babies were tiny and in an incubator. Velker and her husband didn’t know if they would have brain damage or if their lungs would develop properly.
“It was very frustrating not being able to hold them or take care of them,” she says. “As a mother, you ask, ‘What can I do?’ And they said, ‘Well, breastmilk really makes a difference.’”
What we learned about breastfeeding in medical school was, ‘Here is the breast. Here are the different parts of it. This is the hormone that causes it to happen. The end,’ which is basically nothing.
Velker made it her mission to pump breastmilk for her babies. But, like many moms of babies born early, her milk supply was low. Her doctors and the hospital staff were supportive, but no one seemed to know how to boost her supply. A lactation consultant told her that she likely wouldn’t make enough, without offering any tips to make it easier. One nurse said that she would probably give up eventually and just give them formula. Velker was pumping for hour-long sessions, 12 times a day, and getting less than two hours of sleep per night.
“What we learned about breastfeeding in medical school was, ‘Here is the breast. Here are the different parts of it. This is the hormone that causes it to happen. The end,’ which is basically nothing,” she says.
So, Velker, who also holds a Ph.D. in biochemistry, decided to learn everything she could about breastfeeding. She talked to everyone she could find who had a premature baby or who pumped their breastmilk, and read “every mom’s blog” out there. She also started taking domperidone, a drug that increases milk supply, along with any herbal supplements that she read might help. “Inadvertently, I became an expert in breastfeeding and pumping not because I wanted to in medical school, but because I decided to for my own kids.”
She says the real turning point came after she was connected with a doula who is also a lactation consultant. The doula visited her at the intensive care unit, and again once the twins were healthy enough to come home. Velker was scared that her babies weren’t getting enough milk, but the doula reassured her that she could stop bottle feeding and just breastfeed.
“She had this incredible calming aura,” Velker remembers. “She helped me position them in a very calm, ‘you’re the mom, your body knows what to do, just go with it,’ way.”
Today, her 4-year-old twins are healthy. But Velker says becoming a mom changed the way she counsels her patients. Before, she was more likely to say, in general, “Do whatever your OB says because they know what they’re doing.” Now, she’ll tell her patients, “Your body kind of knows what it’s supposed to do, and you always have the right to say, ‘I think I’d rather try something else.’”
It’s hard to initially appreciate that most pregnancies are very normal, and that most people will be totally fine.
She also encourages patients to ask why. “If somebody wants to do a C-section, why? If somebody wants to do a pelvic exam, why?” She notes that it’s important for people to trust and listen to their doctor, but hopes that patients feel empowered to ask for more information.
In medical school, Velker says that they were taught how to manage the worst-case scenario. “But I think in doing that, we get a skewed view of how many people have normal pregnancies versus abnormal pregnancies,” she says. “It’s hard to initially appreciate that most pregnancies are very normal, and that most people will be totally fine.”
Being pregnant today means being caught between two sets of narratives, says Dr. Carla Keirns, assistant professor in medical ethics and palliative care at University of Kansas Medical Center, who is also a mom. “If you buy the Mayo Clinic pregnancy book, then it says one thing, and if you buy the pregnancy advice books written by midwifery organizations or the sort of ‘crunchy, granola’ pregnancy magazine that you might find in a doctor’s waiting room, you get completely different advice.”
Keirns has written about how she didn’t understand the pressure to have a C-section until she gave birth to her son. Then, after she published her story in The Washington Post, Keirns found herself trolled by people who claimed she had endangered her baby by not agreeing to a C-section. Scared moms reached out to ask if they might face the same issues. Keirns told them they had to have a doctor they trusted.
Her experience reflects the uneasy split in the advice people get about pregnancy. “I think it’s a disservice that medical school doesn’t at least expose you to the natural childbirth, breastfeeding advocacy, ‘trust-women’s-bodies’ narrative because a lot of women are going to come to pregnancy with that,” Keirn says. “The fact that you either don’t hear about it, or hear it disparaged, in medical training, I don't think is helpful.”
She adds, “It’s hard to find middle ground, reasonable perspectives where you say, OK, I want the safety of a hospital delivery but I want the trust-women’s-bodies approach as long as that’s safe.’”
CORRECTION: A previous version of this article mis-identified Dr. Janet Zhao's professional name. It has been updated.
Check out Romper's new video series, Bearing The Motherload, where disagreeing parents from different sides of an issue sit down with a mediator and talk about how to support (and not judge) each other’s parenting perspectives. New episodes air Mondays on Facebook.