News
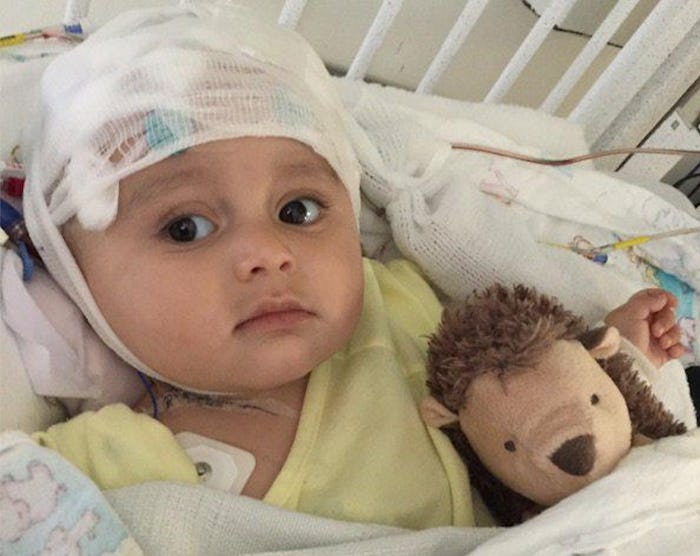
An Insurance Company Reportedly Deemed A Baby's Brain Cancer Treatment "Unnecessary"
Finding out that your baby is sick is easily one of the worst experiences any parent can go through — and the cost of treating their loved one should be the last thing on their mind. When one family in Smithtown, New York, discovered that their infant son had brain cancer, however, they not only had to go through the stress of treating him, but they claim that their insurance company deemed their baby's brain cancer treatment medically "unnecessary" and thus wouldn't be covering it.
When their son, Connor, was around 7 months old, retired New York Police Department officer Wayne Richardson and his wife, Janaida, woke up in the middle of the night to hear him screaming. It wasn't just a usual cry, either — Richardson told the Daily Beast, it was "like when somebody dies." Janaida rushed Connor to the hospital, where doctors discovered he had a brain tumor that was cutting off fluid to his spine. Doctors then did immediate emergency surgery.
"The surgeon told me after we left that he almost lost him on the table," Richardson told CafeMom on Thursday. "He got 85 percent of it and had to stop due to bleeding."
After two more surgeries, doctors at St. Jude Children’s Research Hospital discovered that Connor's tumor — an aggressive teratoid rhabdoid tumor, which is a rare and fast-growing type of cancer — had returned. It had also spread down to his spine.
Doctors enrolled Connor in a clinical trial at St. Jude's. The course of treatment would include one experimental medication along with four other drugs — and to Richardson, the treatment is clearly a necessity. "He’ll die if you don’t do it," Richardson told the Daily Beast. "You don’t care what it costs."
And yet, the Richardsons' insurance company allegedly deemed the treatment "medically unnecessary" in a letter reportedly addressed to Connor himself. According to CafeMom, the insurance company reportedly wrote:
This combination of medications is not the standard of care for this type of cancer, and is considered experimental and investigational at this time, as evidence-based guidelines do not exist to confirm its effectiveness for his brain tumor. Therefore, this request for clinical trial treatment at St. Jude's hospital is not medically necessary and is denied.
HealthCare Partners, IPA did not immediately respond to Romper's request for comment. What it seems to boil down to, though, is this: since the treatment doesn't guarantee recovery or have numbers to prove its effectiveness, the company allegedly won't cover it.
However, even the National Cancer Institute at the U.S. Department of Health and Human Services recommends that patients with Connor's kind of tumor "think about taking part in a clinical trial."
"For some patients, taking part in a clinical trial may be the best treatment choice," reads a National Cancer Institute summary on teratoid rhabdoid tumors. "Children with atypical teratoid/rhabdoid tumor should have their treatment planned by a team of health care providers who are experts in treating cancer in children."
Fortunately for baby Connor and his parents, St. Jude's offered the family treatment free of cost, despite Richardson's estimate that treatment would likely cost around $2 million. Connor has started his chemotherapy. But Richardson acknowledged to the Daily Beast that insurance coverage would help fund doctors' work — and their very necessary research — at St. Jude's.
"You’re taking away from them and their research… because the insurance doesn’t want to pay," he told the Daily Beast.
No family should need to rely on the generosity of their hospital or whether they have sufficient funds in their bank account to treat their child's brain cancer. Ever. To help out, donate to Connor Richardson's GoFundMe page, then make sure you speak up — loudly — about the importance of people getting affordable, reliable coverage, no matter what illness they're fighting.