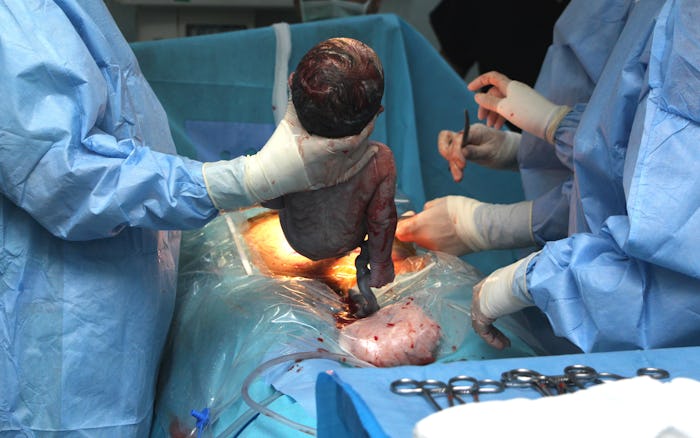
On the day of delivery, the role of an OB-GYN in a hospital setting extends far beyond coaching a mother through the moments of delivery. They are true warriors of the hospital room, ensuring that all is going according to plan — from monitoring the baby’s heartbeat to ensuring the mother is comfortable and that her vitals are precisely where they need to be — and, if necessary, being prepared to alter and change that plan at a moment's notice.
Understandably, it’s a stressful job, but also one of the most rewarding, especially to Lia Wrenn.
Dr. Wrenn, who completed her residency in obstetrics and gynecology at the University of Vermont in 2017 and now works for Affiliates in OB-GYN in Burlington, Vermont, finds her job to be immensely gratifying.
“I think the thing that’s really unique about obstetrics is you meet someone for the first time when it’s the beginning of their pregnancy and then you kind of get to follow them through this whole process. Most people are really excited about having a baby, [especially if] they’ve been trying,” Wrenn says in a phone interview with Romper. “So then to see that whole long process come to fruition in that moment — it’s just so rewarding when people finally get to meet their baby and become a family.”
Aside from her responsibilities at the clinic, Dr. Wrenn is on-call for 24 hours about once every week. Childbirth, although a beautiful process, is undeniably a stressful one that requires much attention and skill. Each mother is different and so, each OB-GYN may have a different perspective throughout the delivery process every time they’re on call. But a typical shift for Dr. Wrenn usually looks like this:
“If a patient calls me and they’re contracting and in labor... they’ll come to Labor and Delivery. Once she gets there, she’s assessed. Usually what the means is we will put the baby on the monitor which will monitor contractions and the fetal heart rate. We’ll get vital signs like her temperature, her heart rate — things like that.
“It’s very patient dependent, honestly, and it kind of depends on what the patient wants. Some patients kind of just want to be on their own and they may have a doula who’s there to support them or their husband is there to support them and they may want things a little more hands-off. And some patients want someone who is a little more hands-on and checking in on them more often.
“I would say, overall, typically we check patient’s progress maybe every two hours to make sure they’re dilating and contracting appropriately. That’s usually a cervical check every couple of hours. If the patient wants an epidural or anything like that, we’ll typically relay that information to the anesthesiology team. We’ll check the patient until they’re completely dilated and then at that point, when the patient is completely dilated, you can start pushing.
We’ll try pushing in different positions and seeing what works for them the most.
“At that point, we’ll push, in the room, typically. We try to make it as least operative as possible and try to make moms comfortable and not like it’s in a medical environment as much as you can.
“We often try — depending on if the patient is able to — we’ll try pushing in different positions and seeing what works for them the most. My other job is to make sure we have a safe delivery. I’m constantly assessing things like if the fetal heart rate is looking OK, is everything going according to plan and, if it’s not, then making another plan for safe delivery, so that would mean either an operative delivery or a c-section.
“After the delivery, as long as the baby is doing OK and looks OK and there’s no other reason not to, we’ll bring the baby immediately skin-to-skin so that mom and baby can have that bonding time. At my hospital, we do something called delayed cord clamping, which is when we allow the umbilical cord to pulse for at least a minute which is thought to kind of give some extra blood to the baby and prevent anemia. And then we’ll clamp and cut the cord. If the dad wants to be a part of that or if there’s another family member who wants to be a part of that, we do that.
It’s super common during your first baby to have what's called a second-degree vaginal tear or perineal tear.
“The second part of the delivery is called the third stage: The placenta delivery. But that’s usually pretty passive for the patient. We’re usually just assessing bleeding and making sure the placenta is coming. And once that’s over, we’ll just check to see if there were any tears, any vaginal tears, during delivery. It’s super common during your first baby to have what's called a second-degree vaginal tear or perineal tear.
“During this entire time that we’re doing this, the baby and the mom are together. We really try to maximize that bonding time. As far as the delivery goes, I will see my moms every morning while they’re in the hospital and we’ll usually have them follow-up in our clinic.
“With any medical profession, I think the hardest part is when you have to give patients bad news. In OB-GYN, lucky, most of our job is happy, but things can be really sad like when a patient has a miscarriage or has a history of miscarriages and then has another one. Or certainly if someone has fetal demise unexpectedly, which is really rare thankfully, but it can be really devastating to tell patients that.
“It’s so gratifying and rewarding because people are just so grateful and thankful. That’s why I went into OB-GYN because I figured if I’m going to be up at 3 in the morning, what would I rather be up at 3 in the morning for? And for me, it’s helping someone complete their family or add to their family with a baby. It just brings so much joy to my life.”
You’ll never forget the birth of your child, but what does everyone else who was there remember? Find out with more from Romper’s look at birth, Stork’s Eye View.