Life
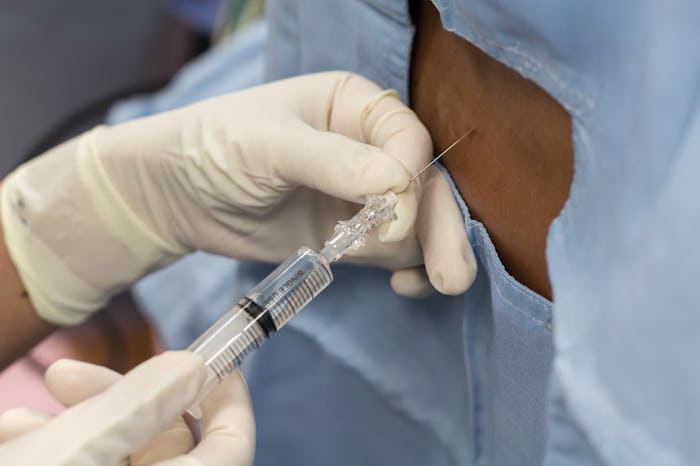
Here's The Difference Between a Spinal Block & An Epidural, So You Can Feel Prepared
When it comes to pain relief, I didn't really give it much thought before I asked for it. I just knew that the unmedicated child birth I had with my son was not something I wanted to repeat. So when the books on pregnancy and childbirth mentioned spinal blocks and epidurals, I was ready to sign up for both. But what's the difference between a spinal block and an epidural? Do you get a choice? Are they specific to one procedure or method of delivery?
They're both regional anesthesias administered via spinal fluid that only block the pain from the point of insertion down, according to The Cochrane Database. However, they're not interchangeable, even though the terms are often used interchangeably in conversation. There is also something that is a blend of the two which is becoming increasingly common called a combined spinal epidural. It's a hybrid of the two that provides all the benefits of a spinal block, while also inserting an epidural catheter into the epidural space, the space between the vertebral wall and dura mater, noted the Carver College of Medicine. This is done so that if more medication is needed, it can be given easily.
A traditional epidural is routinely performed during vaginal birth. Spinal epidurals are a type of regional anesthesia that are given via a catheter that is inserted near the spine after the area has been numbed with a local anesthetic, and the catheter will remain in the epidural space until the epidural is no longer needed. A drip of anesthetic is continually administered via this catheter for the duration of your labor or C-section, according to Heather Nixon, MD. The pros of an epidural are that they last as long as necessary, and if you need more meds after you've given birth, the cath is already in your spine — no need for another painful puncture.
A spinal block, Nixon writes in an email to Romper, is a procedure wherein the injection site is numbed locally, and then a small catheter is inserted into the cerebrospinal fluid in-between two vertebrae with anesthetic injected directly into the fluid surrounding the spinal column. The procedure is quick, and the effects happen in moments. However, it is temporary, with the numbness starting to recede two to three hours after the procedure. It's great for C-sections because the surgery is typically fast and the medication works quickly, although combined epidural spinal block procedures are becoming increasingly more common for C-sections
As far as complications go, Nixon tells Romper, "Common side effects include chills, a drop in blood pressure, and nausea. A small portion of patients (about 1 percent) will experience a headache following spinal anesthesia or epidural catheter placement. This headache may range from mild to quite severe, needing intervention. Major complications include epidural hematoma (bleeding in back), epidural abscess (infection in back), seizures (if medication enters your bloodstream) and nerve injury. Luckily, all of these major complications are very rare."
In the end, it's going to be up to you and your provider to determine the best pain relief for your situation. I've had both, and I'd gleefully get either all over again if I was in labor. It's a balance of need and expectation, like so much else related to childbirth.
Check out Romper's new video series, Romper's Doula Diaries:
Watch full episodes of Romper's Doula Diaries on Facebook Watch.