Life
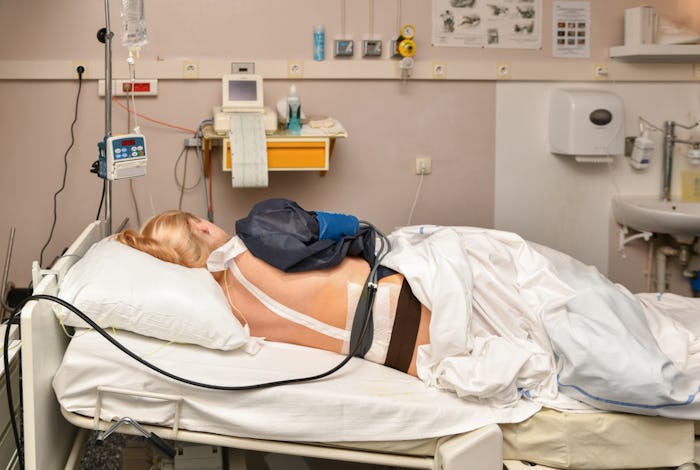
This Might Help You Decide When Exactly You'll Ask For That Epidural In Labor
Being pregnant is, in a word, confusing. For every piece of well-meaning advice you receive, you hear another tidbit that directly contradicts it. "Wait as long as possible to get your epidural so it won't slow down labor," one friend told me. "Get your epidural ASAP. It'll help you relax and speed up the process," a relative instructed only a week later. Wait... so which is it? When is the best time to get an epidural? For moms-to-be who are anxious for pain relief but worried about adverse effects of an epidural, it's imperative to separate facts from fiction.
As it turns out, the idea that an epidural can slow down labor is not just an old wive's tale. However, it's not such a black and white issue, according to L. McLean House II, doctor of Anesthesia and Perioperative Care at the University of California, San Francisco. "The labor epidural can prolong the second stage of labor, and there are many studies which report this," Dr. House says, but it really depends on how much numbing medicine you get. "Lower concentrations of local anesthetic cause less motor blockade, and these dilute concentrations seem not to effect the duration of the second stage of labor." This motor blockade is what makes your legs feel like dead weight. Basically the lower the dose of local anesthetic, the lower the risk of prolonging labor, and vice versa. "Simply express that you want pain relief, but that you don’t want to be 'too numb,'" Dr. House advises Romper. "While standard epidural doses vary by hospital and provider, this may prompt your provider to be more conservative with epidural dosing."
One major concern among mothers considering an epidural is that if labor is prolonged, the need for a cesarean section, forceps, or suction may be increased. However, a 2014 study on the timing of epidural administration disproved that idea. In this study of 15,752 women, Dr. Ban Leong Sng and colleagues found that early initiation of epidural anesthesia (cervical dilation of less than 4 to 5 centimeters) did not increase the need for a cesarean section or the use of suction or forceps compared to the later initiation of epidural anesthesia. For Dr. Sng, the question of when a mom should receive an epidural is pretty simple. "It would appear that the time to initiate epidural analgesia is dependent upon women’s requests," Dr. Sng wrote in her study. In other words, the best time to get your epidural is whenever you choose.
But what about those moms who swear their epidurals actually sped up their labor? They're not lying – but their belief may be based in their own perception rather than reality. If you've ever had a full work day with a migraine or menstrual cramps, you're probably aware of how pain and discomfort can make time slow down. During painful contractions, it can feel like time actually stops. As Dr. House explains to Romper, the epidural may simply make the passage of time easier on laboring moms. "Epidural analgesia does not hasten cervical dilation or ripening, but it certainly takes the edge off of pain," Dr. House tells Romper. "When the relief from the epidural comes, oftentimes expectant mothers rest or nap. Meanwhile, the cervix continues to dilate, and when the patient is 'complete,' then it’s time for more pushing. The anecdote likely comes from an altered sense of the passage of time." I don't know about my fellow preggos, but I'm all for "speeding up time" with an epidural while I'm in labor, even if it's only in my head.
While the "best" time to receive an epidural varies by patient, there is a point of no return when it comes to receiving the pain relief. As my own mother likes to remind me, I came too quickly for her to receive an epidural and she birthed me unmedicated, much to her dismay. When exactly is it too late to receive an epidural? Dr. Leif Dahleen previously told Romper, "A labor epidural does take a little time to set up and give optimal pain relief. If your cervix is fully dilated and you feel ready to start pushing, you've missed that window for an epidural."
Of course, like any medical procedure, epidural anesthesia is not without any risk, and moms choosing to go this route should be aware and informed about them. Dr. House reviewed the various risks with Romper: one in 10 to 20 epidurals have to be replaced during labor because of inadequate anesthesia; one in 100 to 200 epidurals can cause a post-dural puncture headache (a severe headache caused when spinal fluid leaks through the injection puncture site, according to Mayo Clinic); finally, less than one in 80,000 epidurals can cause injuries that persist months after placement. Additionally, women with certain health issues, like thrombocytopenia (a deficiency of platelets in the blood) and coagulopathy (disordered blood clotting), may not be candidates for a labor epidural. It's important for pregnant women to discuss risks and options with their OB-GYN and anesthesia provider.
Nothing about pregnancy is one-size fits all. Every experience varies woman to woman, all the way from conception to delivery. The best time for one woman to get an epidural is not necessarily the best time for another, and figuring out that "sweet spot" ultimately comes down to what you, and your doctor, decide.
After a very frustrating first birth experience, this Deaf mother wanted a change. Will the help of two Deaf doulas give the quality communication and birth experience this mom wants and deserves? Watch Episode Four of Romper's Doula Diaries, Season Two, below, and visit Bustle Digital Group's YouTube page for more episodes.