Life
11 Questions I Should've Asked My OB-GYN Before My Vaginal Birth
Before I had my first baby I was nothing short of nervous. In order to prepare to the best of my ability I took classes, wrote a detailed birth plan, and armed myself with as much knowledge as a soon-to-be mom could handle. As a result, I truly thought I knew everything there was to know about vaginal deliveries. I was wrong. Turns out, there were so many questions I should've asked my OB-GYN before my vaginal birth.
Little did I know, there were a lot of topics my birth class overlooked or downplayed. And, sadly, that very same birth class shamed certain labor and delivery decisions, like getting an epidural. So I had no idea that, when the time came, it would be difficult to advocate for myself when I was experiencing back labor. I also didn't think to ask about scenarios that people don't necessarily plan for, like if your labor doesn't progress or if you need to be induced. I had no idea what to expect after my baby was born, either, like whether I would get a chance to hold my baby immediately after birth, what the hospital's policies were on breastfeeding, and what immediate treatments would be administered to my baby once they were born.
Every provider and every hospital has a different set of rules and protocols to follow when a woman is experiencing childbirth, including who is and isn't allowed in the room during labor and delivery, if the laboring mom-to-be can move freely during labor, and what positions a pregnant woman can labor in. So while I thought I was as prepared as possible, it didn't take me long to realize that there are a set of questions every pregnant woman should ask her OB-GYN to prepare for vaginal birth... and I didn't ask them soon enough.
"How Will I Know If I'm In Labor?"
My midwife kind of chuckled when I asked her how I would be able to tell the difference between Braxton Hicks contractions and the real thing. She replied, "Hh, you'll know." She was right, but it would have been helpful to have some telltale, well described differences in mind so I wouldn't constantly be second guessing myself.
"Is There A Time Limit For Labor?"
Before I had my first baby, I heard that there was a time limit for how long a person could be in labor before they had to be induced. Before I had my last baby, I asked my OB-GYN to set the record straight. It's true that different providers have different protocols to reduce risk of infection and help make sure you and your baby stay safe. For example, mine recommended induction after 24 hours of your water breaking. According to the American College of Obstetricians and Gynecologists (ACOG), the jury is still out about whether imposing time limits on labor or simply "watching and waiting" is the best option for most women.
Because there are risks of infection it's recommend that you head to the hospital if your water breaks. It's also always recommended that you call your provider if you think you're in labor, so your individual situation can be assessed.
"Will I Go Into Labor On My Own?"
There's no way for your OB-GYN to answer this question. Due dates are estimates, and as Parents reports only five percent of us actually give birth on our due dates. I watched my due date come and go, and then finally agreed to induction right before I hit 41 weeks.
Contrary to popular belief, all pregnant women won't go into labor on their own, and after 39 weeks your risk of pregnancy complications goes up rapidly, so you should definitely talk to your doctor about what happens if you don't have your baby by your due date.
"Is There Any Way To Prevent Tearing?"
I think most moms-to-be wonder whether or not their vagina will be the same after delivery. For example, is tearing or an episiotomy an inevitability , or can they be prevented? When I asked about this very question during a prenatal appointment, my provider told me that a research review found that regular perineal massage starting at 35 weeks of pregnancy can make a big difference in whether or not you tear or have to have an episiotomy, especially if you are a first-time mom. It can also help reduce the amount of pain you feel after birth. I only had a tiny superficial tear when all was said and done, so I think giving a perineal massage a shot is more than worth it.
"Who Can Be In The Delivery Room?"
I've birthed at three different hospitals, with three different sets of rules about who was allowed in the delivery room. I definitely suggest you check with your doctor or midwife ahead of time, so you can avoid any uncomfortable conversations. The nurses had to send my parents to the waiting room and, well, that wasn't the best experience.
"What Are My Options For Pain Management?"
When I was pregnant for the first time I was too ashamed to ask my OB-GYN about pain management during labor. I thought I had to at least try for a non-medicated birth. That turned out to be a huge mistake, because advocating for yourself and a change in your birth plan, especially when you're in pain and exhausted, isn't easy. So the last time I gave birth I made sure to ask about my pain management options. I didn't want to be stuck waiting for an anesthesiologist or pain medication because there wasn't an order in my chart.
"When Should I Go To The Hospital?"
While doctors used to recommend heading to the hospital as soon as you experience the first signs of labor, their recommendations now vary based on a variety of factors. ACOG now suggests that laboring women stay home until they reach four to six centimeters dilation and unless they need to be monitored for health risks.
My OB-GYN said to call if contractions got intense, I experienced bleeding, or if my water broke. Because I went to the hospital right away with my first, I ended up getting sent home twice because I wasn't dilated enough for the hospital to admit me for delivery.
"Can I Move Around During Labor?"
In my experience, most providers encourage laboring people to move around as much as they want to during labor, unless there's a medical reason — like an epidural and catheter or a complication — that makes that impossible. The second time I was in labor, the nurse encouraged me to drag my IV along with me through the hallways to help manage my pain. It wasn't pretty, but it helped.
"What's The Best Position For Pushing?"
According to ACOG, the best position for pushing is the one where you are most comfortable — standing, side-lying, sitting, kneeling, or squatting. Some laboring women might need to try a variety of positions in order to coax their baby into the world.
"What Birthing Tools Do You Have & What Can I Bring With Me?"
I spent my last two weeks of pregnancy bouncing on an exercise ball willing my baby to be born. It never occurred to me that the hospital wouldn't allow me to bring my birthing ball with me, though. So after I brought it into my delivery room my husband had to take it back outside and to our car. The same hospital didn't allow candles, essential oils, or other scented products either, and I had to wear socks when I was in the room. It definitely would've been nice to know all of that beforehand.
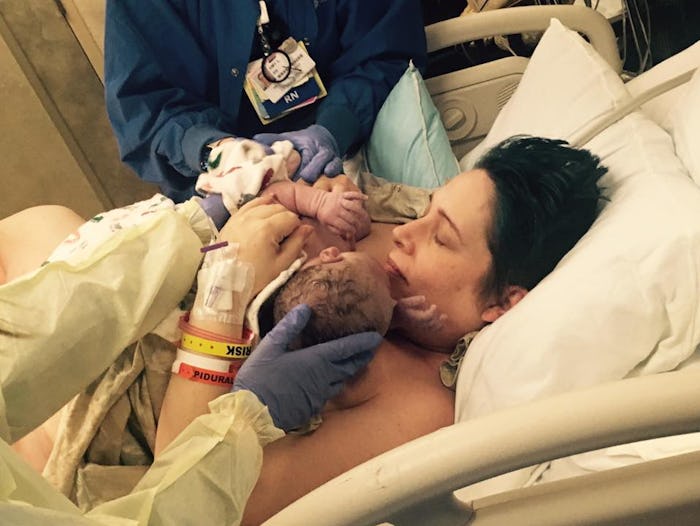
"What Happens After My Baby Is Born?"
I had no idea the hospital where I delivered would want to kick my baby and I out of our delivery suite within minutes of delivery. As a result, I didn't get the "golden hour" of bonding I had hoped for. I wish I had asked beforehand so it wouldn't have felt so awkward and rushed, especially at a time when I was utterly exhausted and needed to take a beat before I started moving around.