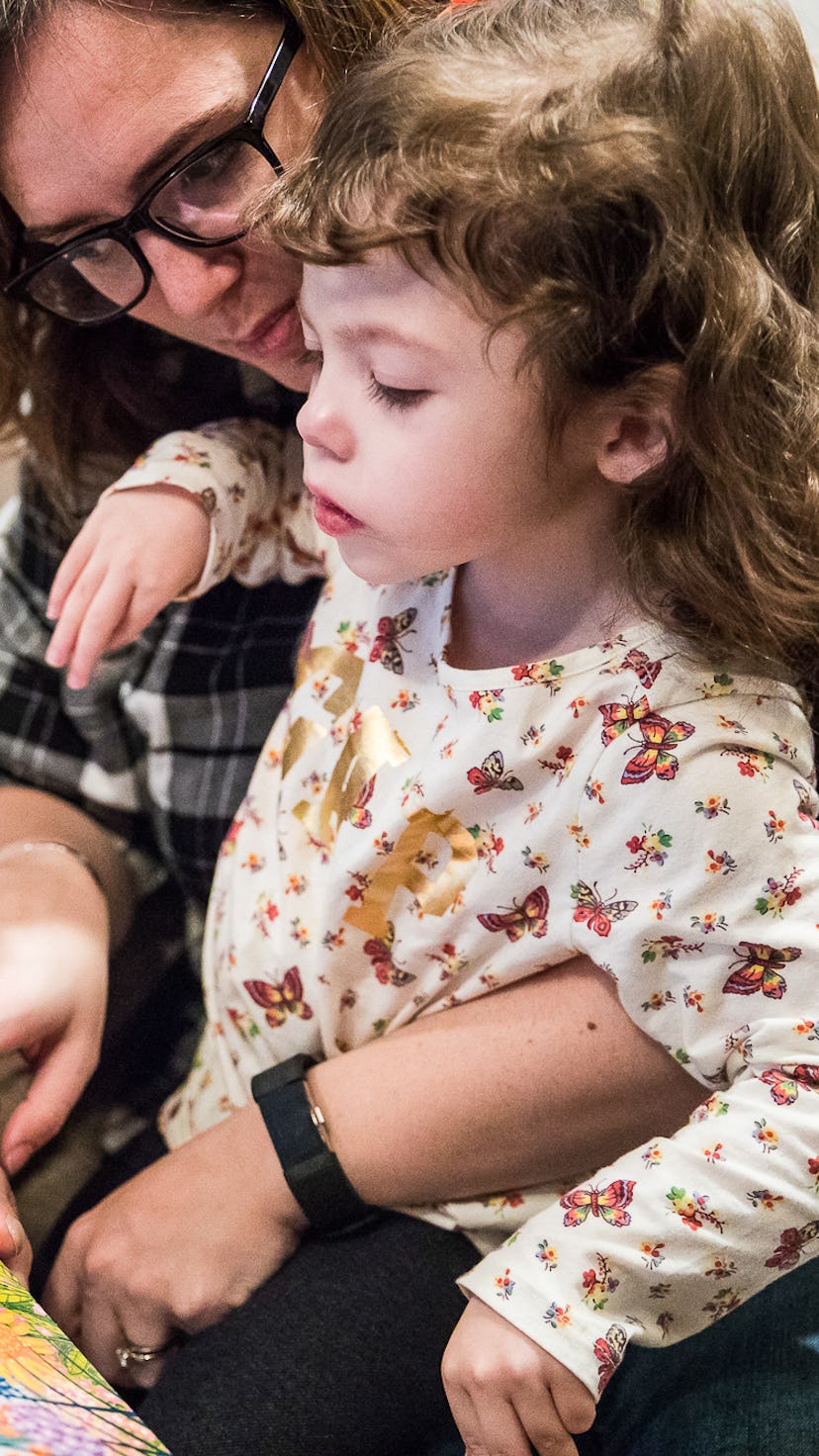For families with medically complex children, each day is a story of survival. Parents' lives are entwined with the medical system that keeps their children alive, and yet go unrecognized by that system when it comes to identifying and treating the ongoing effects of trauma and uncertainty. This Changes Everything goes inside the lives of six families to look at the prevalence of PTSD among caregivers, and consider the steep costs we demand of those fighting day in, day out for their families.
Mackenzie Wardrope lives in Avingdon, Maryland, just outside of Baltimore, with her husband, Greg, and daughter, Adelaide. Adelaide is 4 and has a mutation in the gene SCN8A that leads to epilepsy, developmental delays, and a movement disorder. This is her story, as told to Hillary Savoie.
My daughter Adelaide — we call her Addy — has what's called SCN8A epilepsy. She has major developmental delays. She has seizures fairly regularly. She has a bunch of other complications due to her epilepsy. She has neutropenia, which basically means she has no immune system. She has a G-tube [a surgical opening through her abdomen into her stomach used for feeding] because she does not have the appropriate skills to eat or drink. We diaper her everyday. She cannot stand or walk. She can sit but kind of wobbly. We do pretty much everything for her. She really doesn't have any independence whatsoever. She is nonverbal.
It started with her very first seizure. We did not know at the time that it was a seizure. She was six weeks old, everything had been perfect up until that point. I was feeding her and I was going to put her in her crib, then for whatever reason that day I decided I was not going to put her in the crib. I just wanted to cuddle with her for a few extra minutes. So, while I was holding her, I suddenly felt her go completely rigid. I had no idea what was going on. I looked down at her and she was completely stiff, her eyes were bugged open. Her lips were purple and she was gray. And she was just kind of stiff and not really breathing. I kept screaming her name and she was not responding. My husband, Greg, happened to be home that day sick from work, so I went to the bedroom and I got him.
We called 911. They proceeded to tell Greg to perform CPR on her. I was just in a complete state of shock. I really just didn't know what was going on. 911 stayed on the phone with us until they arrived.
There were two ambulances, a fire truck. There were at least two cop cars that came. In the meantime, my daughter is still not really breathing well and having these jerking motions. The [paramedics] took her out of Greg's hands and put her in the ambulance. And the next thing Greg and I knew we were sitting in the driveway. And they just left. But they didn't tell us anything; they just left.
We just kept asking them, 'Is she OK? Is she's going to be OK?' And they said, 'We can't answer that.'
We got to the hospital. And we were in complete shock. She was still having this ridiculous activity that nobody could put their finger on. And they the doctors couldn't tell us anything. We just kept asking them, “Is she OK? Is she's going to be OK?” And they said, “We can't answer that.”
About 45 minutes after all this had begun, it had stopped. But they didn't know what was going on. So, they decided to airlift her to the hospital in the city. So, Greg went on the helicopter with her.
[At the hospital] they called her the million dollar kid because they did test after test after test. MRI came back normal. CAT scan came back normal. They did a first genetic test there and it came back normal. She was in the PICU (Pediatric Intensive Care Unit) for a week. I could not hold her because she was hooked up to IVs. They put an EEG on her and they found nothing.
So we were in the PICU for six days and getting ready to go to the [regular pediatric] floor, and I had been out in the hallway telling my best friend that we were going to the floor, and then Greg came out and said that she had had what appeared to be a seizure. And the doctors and I specifically remember the neurologist that was on call at the time had said that it was “striking” because they had never seen anything like that on a child that small.
They put her on some medicine and sent us home saying, “Don't worry, probably will never happen again, you know if it does though, videotape it.” Because you know that's what you want to do to your itty-bitty little baby, that's your main concern. We were sent home, and we were terrified.
For the first few months she was back in the back in the hospital, because she was constantly having these seizures. The EMS pretty much knew her by name just by our 911 call.
While we were hospitalized one time, they came into our room and told us we had 20 minutes to make a decision on what medication we were going to proceed with next. I did not know my ass from my elbow when it came to medicine.
[When Addy was 6 months old], I had gotten a phone call, I was at my aunt’s in Brooklyn, and the resident called to tell me Addy’s diagnosis [of an SCN8A mutation]. At that point, there were only 12 documented cases of SCN8A in the world. And she told me that Addy would either die during a seizure or she would be severely mentally handicapped. She said this on the phone. And I told her not to label my kid and that we would figure out how to navigate one step at a time. And of course, she said, “Don't Google.” And that's what I did, as every parent does.
That's how I stumbled upon the support group. And I think for a time there might have been 20 members in the support group. Juliann [Bradish, who runs the SCN8A support group] was a pharmacist and had a head start on where we were in the process. While we were hospitalized one time, they came into our room and told us we had 20 minutes to make a decision on what medication we were going to proceed with next. I did not know my ass from my elbow when it came to medicine. And so, I had asked Juliann to call me and she did. And she had told me to focus on sodium channel-blocker drugs. So, I had relayed the message to the team and we have gone forward with those in hopes that things would magically stop.
And that was all in the first year, things kind of got like stabilized, a little bit. But we had a lot of issues with our doctor. He was not going to work with any other SCN8A doctors. He kind of went on his own agenda. So when we had gone to the first Cute Syndrome Foundation gathering, I had spoken about Addy at the conference. After I did my speech, Dr. Mandy Harris came up to me. She had said, “If you ever run into any problems, I'll be happy to help your pediatrician until you find somebody, but you need somebody that's going to help you.”
We ended up going out to Indianapolis [to see Dr. Harris] because we were desperate. We drove to Indianapolis — we can't fly because she has neutropenia. And we saw [Dr. Harris]. It was wonderful and she was so on top of, like, “Okay, this is what we're going to do.” We had a game plan, she wrote a letter of medical necessity, she wrote an action plan out for us. She gave us a list of tests to get done. She called to see if we could do an ambulatory EEG. She called different areas and got an oxygen supply. And she did everything to make sure we had what we need, because she really knew what was going on with SCN8A research. And she just was very informed, so that was wonderful.
[We found a wonderful local neurologist] and we finally got to see him in the beginning of March 2017. And then on March 16, Addy ended up seizing completely out of control and ended up being admitted to the PICU. At this point we didn’t know that Dr. Harris had fallen into a diabetic coma because she had type one diabetes.
So, here we are at a brand-new institution and even though we had a great new doctor, our go-to was in the fight for her life. And nobody really knew what to do, because Dr. Harris was our go-to. Unfortunately, Mandy passed after Addy was in the hospital for three weeks at that time. And it just felt like our world just kind of went through an earthquake and there was no light on anymore. Because the one person that cared most about, not just my kid, but our entire community, was gone. And it was incredibly scary. Who now knew the next step in how to help our kids? I mean, there were researchers that have been working on it. But there weren't any clinicians that had that connection like she did. She was always available.
You are waiting for your child to take that first breath to know that they are going to breathe again.
Meanwhile Addy was still in the PICU. She was not doing well. We were having a hard time keeping her drug levels straight. Her seizures were long; they would average 45 minutes. Her seizures were so bad, they ended up causing femur fractures and compression fractures in her spine. Her seizures have been so bad that there have been PICU nurses and doctors that have left her room in tears.
And that's not a good feeling.
And she would [desaturate to] incredibly low [oxygen levels], sometimes hit zero. Which is hard because you are waiting for your child to take that first breath to know that they are going to breathe again. And we kind of held our breath with her because we were just waiting for her to take that next breath, because, again, we just didn't know if she was going to.
I wouldn't take her to the hospital because I didn't want to relive everything over and over again. And I just thought to myself, 'Well if I don't take her, then it is not real.'
What ended up happening was during this four-month period of time, I did not leave her side for a good chunk of it. And I was so incredibly stressed that I developed shingles. Because she doesn't have an immune system at all, she was put on air isolation for 28 days and I could not be around her for a minimum of two weeks because I was carrying a virus. I had to stay home, my husband had to stay with her. He had to. I feel like I don't ever give him enough credit. It was really hard on him, too, because he doesn't really like hospitals, it's a hard place for any parent, but he really struggles with it. And that was kind of my thing and he had to step up and be there and make some really difficult decisions. I was home going out of my mind.
I feel like I have signs of PTSD [like avoidance]. Addy was put in the hospital March 16, and this year as we approached that date, Addy was getting very sick. I was in complete denial. And I didn't take her. I wouldn't take her to the hospital because I didn't want to relive everything over and over again. And I just thought to myself, "Well if I don't take her, then it is not real."
I have plenty of flashbacks of her turning purple and not breathing. I kind of just freeze. I get a little bit panicky. I just get heartbroken for my kid. She's pretty amazing because she goes through she so much. And like I feel like it's almost selfish for me to feel any anxiety over what she's been through because I'm not the one that's going through it. She is.
But there's constant fear. I mean, I have in my head, I have envisioned my child’s funeral, because I know the reality of how sick she can be and how close we've come to that. And it's horrible. There was a family that we met while we were in the hospital. We became incredibly close with them. And they, unfortunately, lost their daughter. And while I was at the funeral, I felt immense guilt because my daughter was still there. But then at the same time I felt like it was a precursor for what's to come. I try to be positive because if I focus on all the negative all the time, it puts you in a really bad place. But it's hard it's hard when your reality is so scary. It's not something that it's like “not my kid” because we’ve seen it happen. And that’s the thought that goes through my head every single day.
If I find myself really dwelling on that, my instinct usually is to immediately pick Addy up and hold her and just try to absorb the moment. But I do try to do a lot of busy stuff. I do like crafting and painting. And I try to go out with friends or a talk with some crazy other moms. You know, it's important to maintain a healthy relationship with other people that understand because you know how to lift each other up. And you all take turns in taking care of each other.
It's incredibly isolating when you have a medically fragile child. I have certainly seen friends and family kind of back off because they don't know what to do. And it's hard because Addy’s still my daughter, she’s still a person. She still has feelings. She still deserves to be loved.
I am very fortunate that my mom and dad, who have their own medical issues, they go out of their way to try and help because I’m their daughter. They see me struggle quite a bit. The friends that have stuck by me, I might not be able to be a friend to them in the same capacity as I have been in the past because my life is different. But there have been friends that have tried to help me that don't have a situation like mine. It takes work. It takes effort. It takes asking questions, being present. People in our situation might be scary sometimes, but you know it's really hurtful when people turn their back and ignore or come up with excuses. There's nothing I can't stand more than coming up with excuses for why you can’t, because my kid deserves better than that.
Honestly speaking, there's a part of me that's really bitter. I mean I resent when you know someone talks about how the hardest day of their life was their kids fell scraped their knee or like needed two stitches in their finger and it was like so traumatic. It's something I struggle with because it’s not their fault but in the same token I'm like: at least your child isn't laying on a PICU table. And you know you aren't counting the seconds hoping that your kid’s going to start breathing again. So in retrospect like: Not so bad for you right now.
I mean it's a terrible thing say, but that's my truth. It's hard. Our lives have changed. And it's a challenge, and you try to keep things in perspective because there is always somebody that wants to be where you are. But it's really hard not to look at somebody else who is farther than you and not want for that as well. And it's not for you; you want [it] for your child.
This interview has been edited for length and clarity.
Photography: Kisha Bari
If you or someone you know is experiencing symptoms of PTSD or a related condition, contact the National Alliance On Mental Illness HelpLine at 1-800-950-NAMI (6264), Monday through Friday, 10 a.m. to 6 p.m. If you are experiencing postpartum depression or anxiety, you can also contact the Postpartum Health Alliance warmline at (888) 724-7240 or Postpartum Support International at (800) 944-4773. If you are thinking of harming yourself or your baby, get help right away by calling the National Suicide Prevention Lifeline at 1-800-273-8255, or dialing 911. For more resources, you can visit Postpartum Support International.