Premature Birth
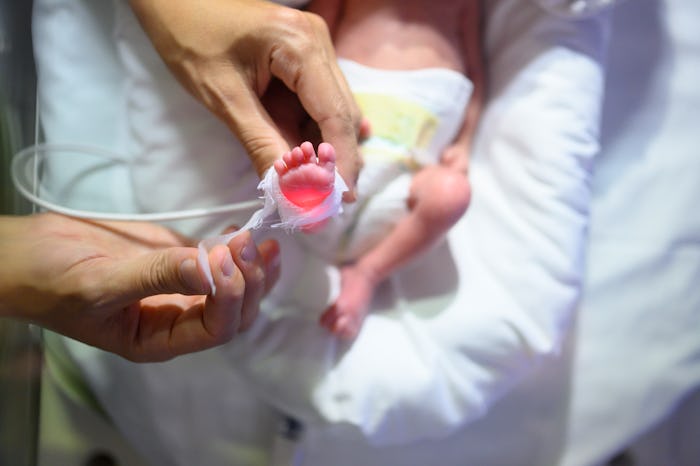
What's A Micro Preemie? These Tiny Soldiers Are Pretty Amazing
A guide to the smallest babies of all.
Premature birth is defined as a baby that is born not just before its due date, but before 37 weeks of gestation. But there’s a subset of infants that falls into an even smaller category within the premature designation. These are micro preemies, extremely premature babies that are born at less than 26 weeks. These babies are measured in grams, not pounds because they are so small and due to their birth weight and size, often require medical intervention to survive and thrive.
However, micro preemies are not a monolith. As Dr. Joanna Parga-belinkie, the Medical Director of Newborn Nursery at the Hospital of the University of Pennsylvania, explains, each micro preemie baby is an individual that requires its own unique course of medical care and attention. This, she admits, can make understanding micro preemie complications all the more confusing for parents and families.
What is a micro preemie?
“I think it refers to babies born less than 26 weeks,” says Dr. Parga-belinkie. “They’re either extremely low birth rate, less than 1,000 grams, which is 2 pounds, 3 ounces. Then it goes up from there to 1,500, which is a very low birth rate.”
What causes premature birth?
“If I knew the answer to that, I’d have a Nobel Prize,” says Dr. Parga-belinkie. The truth of the matter is, science still hasn’t revealed a singular cause for premature birth. What doctors like Parga-belinkie do know is that complications like inflammation or infection can lead to premature birth. “It could also be related to the placenta,” says Dr. Parga-belinkie. “How the placenta is attached to the uterine wall or how it’s providing oxygen and nutrients to baby can cause issues.” And then there’s congenital issues as well that can’t be ruled out. Certain congenital issues can stunt a baby’s growth in utero.
“But we don’t have a consensus or one answer to avoid preterm birth. And that’s what I think is hard for families. It can be kind of nebulous,” she says.
What isn’t nebulous is the care the NICU will deliver for a micro preemie. While Dr. Parga-belinkie says severe cases might require a level 3 or 4 NICU, that is one with a host of surgical interventions and tools, most regional hospitals are equipped to care for a premature infant.
What are the health concerns for micro preemies?
“Chronic conditions can develop as a result of the immaturity of when they were born. But it’s so hard to predict what their development will be,” says Dr. Parga-belinkie.
That said, the National Institutes of Health has a tool to determine the possibility of outcomes for babies born early. This includes profound neurodevelopmental impairment, blindness, deafness, and moderate to severe cerebral palsy, as well as cognitive development delays.
Dr. Parga-belinkie adds that with the right intervention, some micro preemies may not experience any of these complications.
What are the survival rates for micro preemies?
“Each baby is an individual. I look at all the individual stats. What gestational age is this baby? Is it a singleton? Are there others? Is there time to give steroids — to get their full effect, you need to give two doses and hopefully keep mom pregnant for two days — ,” says Dr. Parga-belinkie. “I go through all of the organ systems in those first 24 to 48 hours are critical to survival.” She adds that once a baby has made it past the 48 hour mark, they have a much better hope of survival.
The NIH website, however, offers a Extremely Preterm Birth Outcomes Tool where individuals can input facts about an infant including gestational age, birth weight, etc., and it will produce statistics regarding average survival and hospital range.
Can you breastfeed a micro preemie?
So much of the bonding between baby and parents takes place with touching and holding a child, not to mention breastfeeding for those who choose to do so. However, micro preemies are often intubated, which means they have a tube inserted into their throat to allow them to breathe. This can prevent breastfeeding. However, Dr. Parga-belinkie says that once a micro preemie has developed enough to breath on their own — and if a medical team deems it safe —a birth parent can begin introducing the breast.
“We try to promote breastfeeding in the NICU. So when the baby starts to show a suck reflex, generally at 34 weeks, we try to have that first feeding be at the breast,” says Dr. Parga-belinkie. This might mean that a birth parent has to pump for many weeks while the baby receives their breastmilk (or sometimes a donor’s) via feeding tube. It also might mean supplementing breastfeeding with a bottle of breastmilk that’s been fortified with additional nutrients for optimum growth.
“We try to get all babies on 24 calorie per ounce feedings and usually we estimate that breast milk is about 20 calories per ounce, so we have to fortify the breast milk to give extra calcium and extra phosphorus or nutrients to promote bone health and other things,” she adds.
But even with the need for fortified breastmilk, breastfeeding is highly encouraged for micro preemies when the time is right.
Where to buy clothes for micro preemies?
You might not find the itty bitty clothing needed for your micro preemie at general retailers, but there are options online.
- Preemie Store - this NICU-friendly retailer sells clothing that’s not just small, but designed just for the needs of baby’s undergoing interventions with open shoulders, footless, and easy front access options.
- Preemie Clothes Smart - has a section designed exclusively for babies weighing one to four pounds.
- Itty Bitty Baby Boutique - touts itself as NICU-safe, meaning the clothes have been designed for the various interventions used within the NICU.
Where to buy micro preemie diapers?
The good news is that the diaper industry understands that the littlest babies need moisture protection too. Huggies and Pampers both sell super tiny options. Ordering online is likely the best option as some retailers don’t carry the extra small size.
For parents of micro preemies, Dr. Parga-belinkie will be the first to admit the road ahead may seem daunting. But she urges parents to remember that their NICU team is there for them and wants to work with them for the shared goal of seeing their baby survive and thrive.
Expert
Dr. Joanna Parga-belinkie, Medical Director, Newborn Nursery, Hospital of the University of Pennsylvania (HUP); Attending Neonatologist, HUP & Children's Hospital of Philadelphia (CHOP); and Assistant Professor of Clinical PediatricsCo-Host of Pediatrics on Call by the American Academy of Pediatrics (AAP), jpbelinkiemd.com
This article was originally published on